Healthy and resilient individuals are the foundation of strong communities. Part of the reason our communities are struggling is that people are struggling. Improving our well-being makes us more able as individuals – and as organizations and families made up of individuals – to take good care of each other.
Individuals who consistently practice self-care will bring positive change to their community. The challenge of caring for people during the Covid-19 pandemic can be daunting. Instead of waiting for massive political, cultural, or socioeconomic shifts to happen, we can have a collective impact – made up of individuals committed to caring for themselves so they can better care for each other.
Work of Care offers free tools that support your personal well-being, so you can sustainably care about the people you interact with each day. Empower yourself to change the moment. Change the moment, and you change the world.
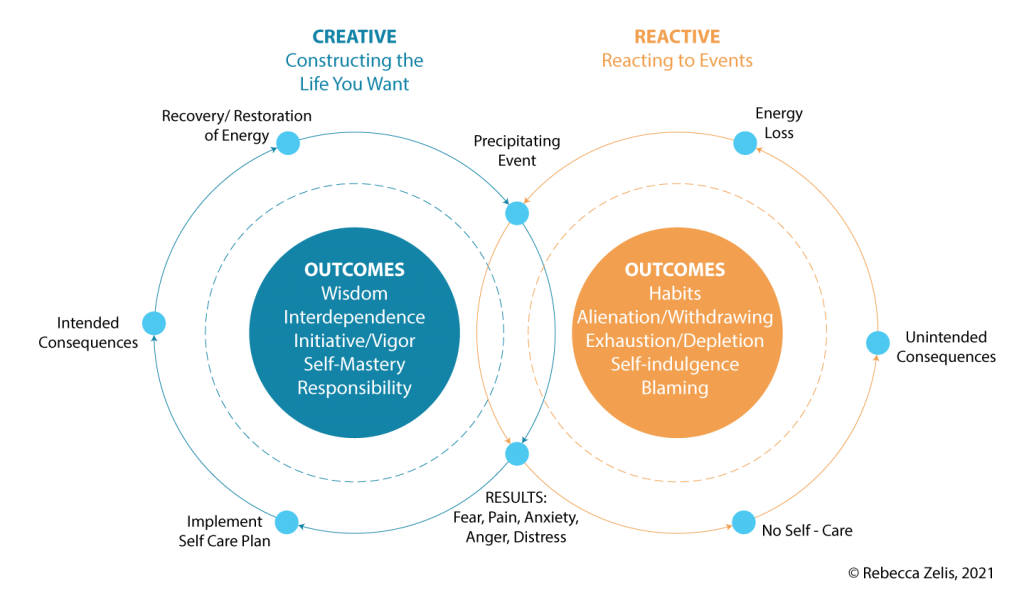
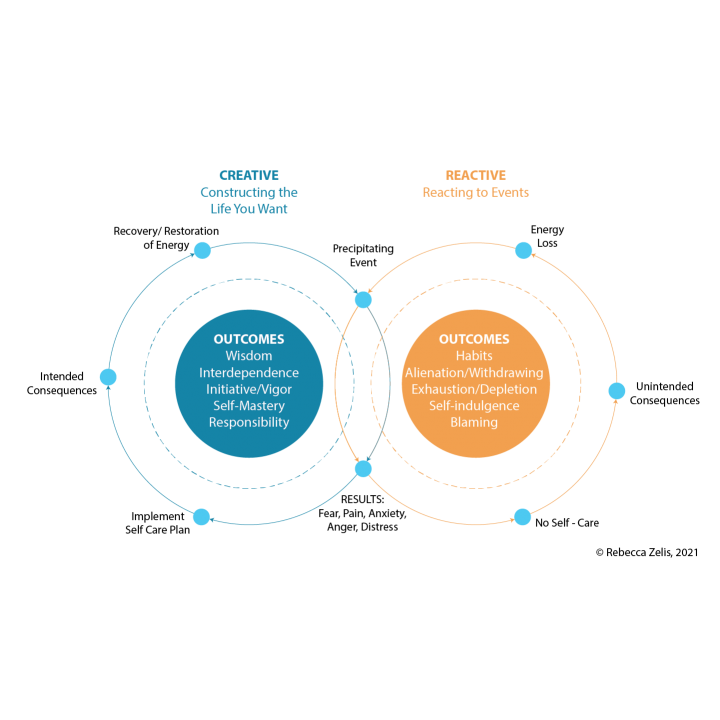
SELF-CARE IS OFTEN PRESENTED AS AN END-POINT, AN INDULGENCE OR ESCAPE FROM DAY-TO-DAY LIFE. WORK OF CARE SUGGESTS SOMETHING DIFFERENT: THAT SELF-CARE IS A STARTING POINT FOR BETTER SERVING OTHERS.

Recent Articles
Your Primary Resources
Assessments, Printable Worksheets & Links

Assessments
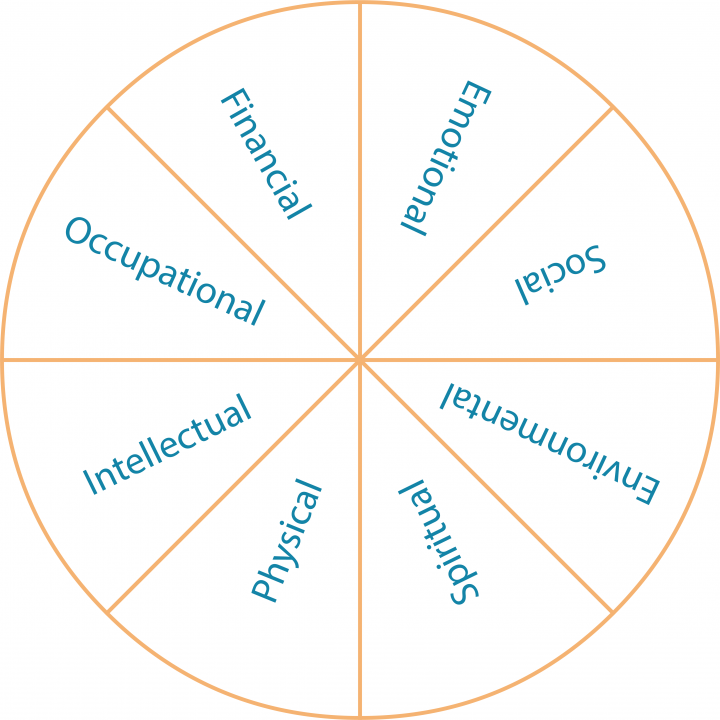
Assessments help to assess how people are doing right now in areas like sleep, home environment, relationships, and other aspects of well-being.

Self-Care Workbooks
Step-by-step resources for self-care, with the goal of building personal well-being so people are better able to do the work of caring for each other.
Organization
Symptom trackers and goal setting charts to support the logistics of self-care.